


  |
 |
Timothy F. Hoban, MD
Assistant Professor of Neurology & Pediatrics
Loyola University Medical Center
Epilepsy represents the most common serious neurologic problem affecting children, with an overall incidence approaching 2% for febrile seizures and 1% for idiopathic epilepsy. Diagnosis is complicated by protean clinical manifestations which are age-dependent and differ substantially from adult seizure disorders. For example, infantile spasms may be misinterpreted as a simple startle reflex and absence (petit mal) seizures are sometimes attributed to inattention or attention deficit. Effective treatment depends largely on the physician's ability to establish an accurate diagnosis and choose appropriate therapy based on the likelihood of clinical benefit as well as potential side effects.
The information contained in these web pages and informational modules is intended for review and general educational purposes only and no guarantees can be made with respect to accuracy, completeness, errors, or omissions of content. Please review the full disclaimer before proceeding.
Childhood seizures represent paroxysmal clinical events characterized by abnormal, excessive discharges originating from populations of cortical neurons and resulting in some clinically evident alteration of function or behavior. Therefore, the clinical manifestations of childhood seizures need not include recognizable motor activity such as tonic-clonic movement; possible clinical manifestations may include staring, drop attacks, behavioral changes, or even autonomic disturbances.
Classification of seizure disorders has evolved considerably over time. Use of such terms as "grand mal" or "petit mal" epilepsy have largely been supplanted by more detailed classifications based on specific clinical manifestations, mode of onset (i.e. focal or generalized) and discrete clinical syndromes.
At present, the epilepsies of childhood are most frequently classified using variations of the International Classification of Epileptic Seizures. This nomenclature delineates seizures in three general categories: generalized, partial (focal), and special epileptic syndromes.
Generalized seizures are thought to originate within the brain in a bilaterally symmetric fashion at onset. Convulsive varieties of generalized seizures may include tonic, clonic, and tonic-clonic moter activity. Nonconvulsive generalized seizures include such varieties as absence (petit mal) and atonic seizures, juvenile myoclonic epilepsy, and infantile spasms.
Partial (focal) seizures begin focally within the brain at onset, although they may subsequently progress to a partially or fully generalized seizure. Simple partial seizures produce no alteration of consciousness despite clinical manifestations which may include sensory, motor, or autonomic activity. Complex partial seizures may produce similar sensory, motor, or autonomic symptoms, but are also characterized by some impairment or alteration of consciousness during the event. It should be noted that this definition does not require complete loss of consciousness as a necessary clinical component for a complex partial seizure.
Special epileptic syndromes include such entities as other myoclonic epilepsies, reflex epilepsies, and febrile seizures of infancy.
The etiologies which underlie the development of epilepsy in childhood vary in an age-dependent fashion. Seizures in neonates, infants, and toddlers most frequently result from perinatal brain injury, congenital central nervous system malformations, and metabolic derangements. Central nervous system infection, genetic epilepsies, and neurodegenerative disorders are more likely to present with seizures beginning in later childhood. These causes stand in stark contrast to the adult population, where traumatic brain injury, cerebrovascular disease, and neoplasms represent the most frequent causes of seizures.
Determination of appropriate treatment for a child with epilepsy must be individualized based on the spcific type(s) of seizure, the child's age, and the likelihood of significant side effects. Anticonvulsant monotherapy is preferred when possible and is effective in a majority of children.
Generalized seizures may be controlled using a variety of medications, including barbiturates, phenytoin, valproic acid, or Ethosuximide.
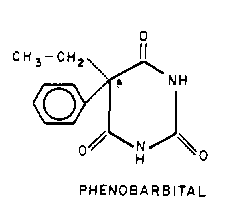 Phenobarbital may be effective in the treatment of both generalized
and simple partial seizures, including status epilepticus. Pediatric maintenance doses
average 3 to 5 mg/kg/day. Common dose-related side effects include sedation and ataxia and
hyperactivity is occasionally evident. Risk for idiosyncratic hepatotoxicity and for rash
is probably not dose related.
Phenobarbital may be effective in the treatment of both generalized
and simple partial seizures, including status epilepticus. Pediatric maintenance doses
average 3 to 5 mg/kg/day. Common dose-related side effects include sedation and ataxia and
hyperactivity is occasionally evident. Risk for idiosyncratic hepatotoxicity and for rash
is probably not dose related.
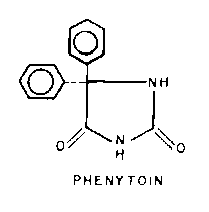 Phenytoin
is also effective in the treatment of both generalized and partial seizures and may be
administered intravenously as treatment for status epilepticus. Pediatric maintenance
doses average 4 to 7 mg/kg/day. Intravenous infusion of a loading dose (18 mg/kg) should
be performed slowly and cautiously due to risk of hypotension. Dose-related side effects
may include sedation and ataxia. Long-term use may be complicated by gingival hyperplasia,
hirsutism, or lymphadenopathy. Potential idiosyncratic side effects include rash,
hepatotoxicity, or a lupus-like syndrome.
Phenytoin
is also effective in the treatment of both generalized and partial seizures and may be
administered intravenously as treatment for status epilepticus. Pediatric maintenance
doses average 4 to 7 mg/kg/day. Intravenous infusion of a loading dose (18 mg/kg) should
be performed slowly and cautiously due to risk of hypotension. Dose-related side effects
may include sedation and ataxia. Long-term use may be complicated by gingival hyperplasia,
hirsutism, or lymphadenopathy. Potential idiosyncratic side effects include rash,
hepatotoxicity, or a lupus-like syndrome.
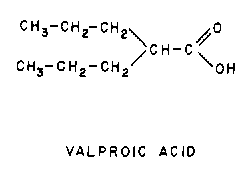 Valproic acid
is useful in treating a variety of generalized (tonic-clonic, absence) and partial seizure
disorders as well as some myoclonic epilepsies. It is particularly useful in treatment of
mixed seizure disorders. Pediatric maintenance doses range from 30 to 60 mg/kg/day PO and
no intravenous form is available. Dose-related side effects may include sedation, GI
upset, thrombocytopenia, and hyperammonemia. Fulminant hepatotoxicity is the most feared
idiosyncratic complication of therapy; children under 2 years of age and children
receiving multiple anticonvulsants appear to be at greatest risk.
Valproic acid
is useful in treating a variety of generalized (tonic-clonic, absence) and partial seizure
disorders as well as some myoclonic epilepsies. It is particularly useful in treatment of
mixed seizure disorders. Pediatric maintenance doses range from 30 to 60 mg/kg/day PO and
no intravenous form is available. Dose-related side effects may include sedation, GI
upset, thrombocytopenia, and hyperammonemia. Fulminant hepatotoxicity is the most feared
idiosyncratic complication of therapy; children under 2 years of age and children
receiving multiple anticonvulsants appear to be at greatest risk.
Ethosuximide is used primarily in the treatment of absence (petit mal) epilepsy and occasionally as an adjunctive agent in other generalized seizure disorders. Maintenance doses average 20 to 30 mg/kg/day. Common side effects include sedation, headache, and stomach upset. Idiosyncratic reactions may include rash or blood dyscrasias.
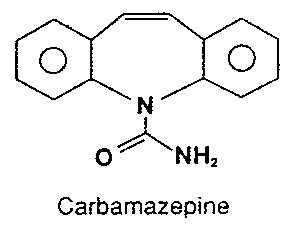 Partial seizures often respond to many of the anticonvulsant medications used for generalized
seizures, including phenytoin and valproic
acid. Another first-line agent used in the treatment of partial seizures is carbamazepine, which is effective against both partial and secondarily
generalized seizures. Maintenance doses average 10 to 20 mg/kg/day PO. Dose-related side
effects may include stomach upset, sedation, and ataxia. Potential idiosyncratic reactions
include leukopenia ,aplastic anemia, rash and Stevens-Johnson syndrome
Partial seizures often respond to many of the anticonvulsant medications used for generalized
seizures, including phenytoin and valproic
acid. Another first-line agent used in the treatment of partial seizures is carbamazepine, which is effective against both partial and secondarily
generalized seizures. Maintenance doses average 10 to 20 mg/kg/day PO. Dose-related side
effects may include stomach upset, sedation, and ataxia. Potential idiosyncratic reactions
include leukopenia ,aplastic anemia, rash and Stevens-Johnson syndrome
| thoban@lumc.edu | Last Updated: August 11, 1996 Created: July 25, 1995 |