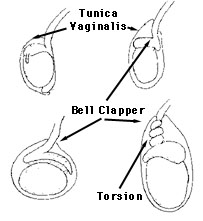
| Failure of normal posterior anchoring of the gubernaculum, epididymis and testis is called a bell clapper deformity because it leaves the testis free to swing and rotate within the tunica vaginalis of the scrotum much like the gong (clapper) inside of a bell. Twisting of the testis on the axis of the spermatic cord is called spermatic cord torsion. The twisting causes edema of the spermatic cord resulting in obstruction of the lymphatic, then venous and finally arterial vessels to the testis. When the arterial supply is impaired, testicular ischemia results. If a boy has had pain and swelling for 8 hours due to spermatic cord torsion, there is a 50% chance that the testis will be lost. Therefore, prompt diagnosis and treatment are very important. |  |
Prevalence: 1/125 males. Torsion occurs most commonly in boys age 13 to 17 years. There is also an increased incidence in neonates. However, it can occur at any age and it is the most common cause of acute scrotal pain and swelling in boys from birth through age 18. It is not clear why spermatic cord torsion, caused by the congenital bell clapper deformity, often occurs years after development is complete.
Diagnosis: Torsion should be suspected in any boy with acute scrotal/testicular pain. The testis and scrotum are swollen, tender and erythematous. Normal landmarks (epididymis) may not be palpable because of the swelling. These same symptoms and signs, however, can be found in males with epididymitis, orchitis or torsion of a testicular appendage. Non-invasive tests (radioisotope testis scan, color doppler ultrasound) have shown a high sensitivity in detecting perfusion to the testis. However, obtaining these tests takes precious time during which the testis may be lost. Therefore, non-invasive tests should be performed in boys with an acute scrotum in whom torsion is not deemed likely.
Treatment: urgent scrotal exploration. If the testis, when untwisted, shows signs of perfusion, scrotal orchiopexy is performed by placing three permanent sutures to anchor the testis to the deep scrotal layers, preventing further twisting. If the testis shows no perfusion, orchiectomy should be performed. Because the defect can be present bilaterally, the contralateral testis must also be anchored.
Return to Abnormal Testis Development
Return to Normal Testis Development
Return to G/U Development home page.
©David A. Hatch, M.D., 1996