![]()
If a hospital is to manage exposed or contaminated individuals, preparations should be made for such an event. First, a treatment area should be identified. This area should be known and readily accessible by all ancillary services in the hospital. The treatment facility should be in an location where treatment of life threatening injuries can be performed. An area of the emergency room is usually designated to be the Radiation Emergency Area or REA. Although some facilities use the morgue as an REA, the surroundings are not comforting to the patient or relatives. Necessary equipment may not be available, and ancillary services are not as well aware of the morgue location. The media, if they become involved, may make unwarranted assumptions based on the location of the patient.
Ideally, the REA should have a separate entrance from the emergency room so as to not effect the throughput of other patients. This, however, is not an absolute necessity. Access to the REA should be limited to the staff that will be in direct contact with the patient. The REA is considered to be a contaminated area. Anyone entering it should be in protective clothing as if they were dealing with a septic case. No staff should leave the REA without a total body check for contamination. As it may take 10 to 15 minutes for a total body check, repeated entering and leaving of the scene should be discouraged. Staff should be assigned to stay in the room until patient care is complete.
An area outside the REA should be designated as a buffer zone. Within the buffer zone should be a cart or cabinet that contains whatever special equipment may be needed for radiation accident management. Access to the buffer zone should be limited to a nurse or other ancillary personnel directly involved with the care of the patient. This area is to be considered potentially contaminated. The buffer zone nurse acts as a link to the rest of the emergency department and relays special needs such as portable x-rays, fluids, equipment or medications. This nurse also documents the care given to the patient, the levels of contamination present, and efforts made with regard to decontamination. This area should be secured to prevent staff and the public from inadvertently becoming contaminated.
If time permits, the REA and buffer zones should have the floors covered with a sheet of protective material. Herculite is a thick plastic material that is impervious to water. Floor coverings are not absolutely necessary, but they do facilitate later clean up. Traditionally, yellow covering is used for the REA and green for the buffer zone. Plastic garbage can liners should not be used for floor covering. They are slippery and may cause accidents. Similarly, sheets tend to bunch up and make movement difficult. The absorbent nature of sheets makes management of contamination difficult. It is impossible to clean up without removing the cloth sheets. Stepping on a contaminated area may promote transfer to another area of the REA as well.
View the Loyola REA setup variations for between 1 and 10 patients.
Staff preparations are straightforward. The staff that come into contact with the patient should be protected from the possibility of contamination. This is easily done by wearing two layers of standard surgical gowns and gloves. Two layers is recommended because of the ease in removing the outer layer should it become contaminated. The drawback is that the staff may become uncomfortably warm from wearing so many layers. Plastic shoe covers are useful to protect footwear from becoming contaminated. Below note a diagram of proper gowning to receive a contaminated patient.
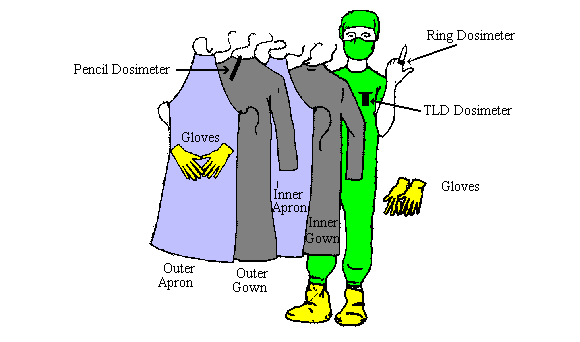
Dosimetry is issued to all staff entering the REA. This applies even to those individuals who may have their own dosimetry such as nuclear medicine technologists or physicians. The purpose of the dosimetry is to document the exposure during the patient management. A thermoluminescent dosimeter (TLD) is worn on the innermost layer of clothing beneath the surgical gowns. A ring dosimeter (optional) may be worn on a finger under the gloves. A pen dosimeter is worn on the outer surgical gown. The TLD and ring dosimeter provide legal records of exposure. The pen dosimeter can be read by the staff member at any time to make them aware of their exposure up until that time. Pen dosimeters however are sensitive to vibration and shock, and are thus not an accurate means for evaluation of exposure.