li-10-2
DISORDERS OF HEPATIC SINUSOIDS by Dr. E. Orfei
-SINUSOIDS IN HEART FAILURE (Right heart failure; Left heart failure):
2-SINUSOIDAL OBSTRUCTION
3-SYNUSOIDAL DILATATION WITHOUT PELIOSIS
4-ANGIOMATOUS LESIONS
5-PELIOSIS HEPATICA
1-Sinusoids in heart failure
Central circulatory failure is due to either right heart failure causing increased pressure in the inferior vena cava or is due to left heart failure causing reduced peripheral arterial blood flow
In the hepatic arteries. The damage in the liver is different.
Rright heart failure
.There will be increased pressure in the inferior vena cava, which is transmitted to the hepatic veins. The sinusoids at the center of the lobule, zone 3, will be markedly congested. The liver cells in this zone will suffer necrosis due to hypoxia and mechanical damage. The patient will have jaundice and elevated serum transaminases.
Left heart failure.
There will be a low systemic blood pressure. The sinusoid in the center of the lobule will not be congested, but the
hepatocytes in zone 3 will be necrotic, coagulated. There will be no inflammatory reaction. The patient will be jaundiced and will have elevated serum transaminases.
Both clinical pictures mimic hepatitis. Both conditions may occur in an acute or chronic form depending on the cause of the heart failure.
Acute circulatory failure may lead to death. Chronic circulatory failure may cause fibrosis and cirrhosis of the liver. Cardiac fibrosis consists of centrolobular fibrosis, which may progress to central-central bridging fibrosis, and lately to central-portal bridges and cirrhosis with regenerative nodules. Cardiac fibrosis is very frequent in chronic heart failure especially in its initial centrolobular stage. Cardiac cirrhosis is very rare, probably because the patients die before reaching that stage.
 |
Fig. 10-2-3 Centrolobular congestion in acute right heart failure. Microscopic changes Notice sinusoidal dilatation and marked congestion with hepatocellular necrosis in the centrolobular area.
|
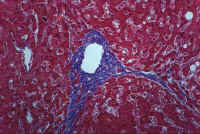 |
Fig. 10-2-3A. Cardiac fibrosis. Marked dilatation and fibrosis of the central lobular vein with formation of fibrous bridges toward other lobules.
|
2-Sinusoidal obstruction.
Is due to reduction of the sinusoidal lumen by swelling of sinusoidal and perisinusoidal cells or by obliteration of the space of Disse by deposition of foreign material such as amyloid. The causes are:
-swelling of hepatocytes
such as in hepatitis, fatty infiltration of hepatocyte, etc.-swelling of Kupffer cells
in storage diseases,(Gaucher, Hurler etc.)-swelling of Ito cells
in hypervitaminosis A.- perisinusoidal fibrosis
obliterating the space of Disse as in cirrhosis.-deposition of foreign material in Disee’s spaces:
amyloid, light-chain gamma globulins.- agglutinated red cell and fibrin thrombi
in sinusoidal lumen: sickle cell crisis.-compression of sinusoids
by nodular regenerative hyperplasia of liver parenchyma.
All these conditions affecting the sinusoids will result in reversible or irreversible
sinusoidal portal hypertension
as opposed to:pre-hepatic portal hypertension
caused by obstructive disorders of the portal vein andpost-hepatic portal hypertension
caused by obstructive disorders of the hepatic veins.
3-Sinusoidal dilatation without peliosis.
It has been reported in association with anabolic and contraceptive steroids in the periportal region. (Winkler K, Paulsen H, Scand . J. Gastroent. 10:699, 1975; Scully R E, New Eng. J. Med.,307:934, 1982).
4-Angiomatous lesions
resembling hemangiomas occur in hairy-cell leukemia.
5-Peliosis hepatica.
Sinusoidal dilatations forming large blood cysts scattered throughout the liver, grossly visible, measuring up to more than 1 cm in diameter. This alteration is not unique to the liver. It may affect other organs with sinusoidal circulation. It has been reported in the spleen, endocrine organs (parathyroids) and may affect even lymph nodes.
The blood cysts in the liver are of two types: the "parenchymal" type not lined by endothelial or Kupffer cells with the wall consisting of an uninterrupted thin layer of reticulin fibers, and "phleboectatic" type, lined by endothelial cells. They appear to represent an exaggeration of sinusoidal dilatation. They may cause no symptoms but when they are large and numerous they may cause jaundice, hepatic failure and may rupture and cause death by hemorrhage.
A peculiar type of peliosis exists in patients with AIDS. Here, the blood cysts are surrounded by a fibromyxoid stroma, which contain locules filled with bacilli stainable with Warthin-Starry stain like the bacilli of cat scratch disease. This type goes under the name of "bacillary peliosis hepatis". The lesion is similar to "cutaneous bacillary angiomatosis" of the skin also seen in patients with AIDS. The bacteria in these lesions are sensitive to antibiotics, which will make the peliosis disappear.
Causes of peliosis: drugs, especially steroids (contraceptives, antineoplastic), metals (copper, arsenic), debilitating infections (tuberculosis, endocarditis AIDS), solid tumors, myeloproliferative disorders (myelofibrosis, polycythemia vera), lymphomas, myeloma, renal transplantation.
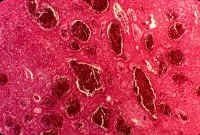 |
Fig.10-2-4-Pelosis hepatica. Presence of large blood cysts, scattered throughout the pulmonary parenchyma, apparently the result of excessive dilatation of single sinusoids.
|
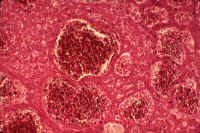 |
Fig. 10-2-5 Peliosis hepatica. The large blood cysts are not lined by endothelial cells. In this case the peliosis is "parenchymal type".
|