 |
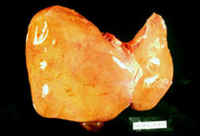
Fig.8-4-1:Fulminant
halothane Hepatitis.
The liver is flabby, soft, friable similar to any acute viral hepatitis. It was called in the past "acute yellow atrophy".
|
|
Li-8-4 DRUG-INDUCED LIVER INJURY by Dr. Emilio Orfei |
INTRODUCTION
Hundreds of drugs are hepatotoxic. We know the mechanism of action on the liver only for few drugs. They attack this organ at different sites. The hepatotoxicity is produced through two mechanisms: toxic metabolites and immunological reaction. Indeed some drugs will continue to damage the liver after their suspension.
Many drugs of every pharmacological group are involved. When a drug reaction is suspected, the literature of administered drug must be reviewed.
PATHOLOGY
Each drug produces different morphological and functional alterations an therefore different clinical manifestations. The morphologic lesions are:
-Hepatitis
, acute, subacute and chronic, indistinguishable from viral hepatitis with hepatocellular necrosis, inflammation, cholestasis. It can be acute and sometimes hyperacute and fatal (fulminant) or it can be chronic with fibrosis and even cirrhosis. Observed with: Amineptine,Nitrofurantoin, Phenybutazone, Quinidine,Sulphonamides.and many more.
-Cholestasis
without inflammation or necrosis. The cholestasis is intralobular, cytoplasmic and canalicular mostly of zone 3. It is attributed to impairment of bile secretion from the hepatocyte into the bile canaliculus for an acquired defect of the bile secretory apparatus of the hepatocyte similar to the congenital defect in Dubin-Johnson syndrome. The prognosis is good with suspension of the drug. Sometimes resumption of the drug after some time does not cause any more the cholestatic reaction.Drugs involved:
Oral contraceptives, estrogens, anabolic steroids. Chlorpromazine.-Cholestasis with portal inflammation
. Changes similar to previous cholestatic picture plus non-specific portal inflammation..Observed with:
Captopril, Azothioprine, Chlorpromazine, Gold, Cyclosporine, Erythromycin, Penicillamine..
-Cholangitis( affecting portal bile ducts) and Cholangiolitis(affecting portal bile ductules).The mechanism is probably immunoallergic. There is epithelial degeneration of bile duct epithelium, neutrophlic infiltration in and around bile ducts or ductules, portal lymphocytic and eosinophilic reaction The lesions are usually reversible with discontinuation of the drug but permanent rarefaction of bile ducts may result with some drugs with changes similar to primary biliary cirrhosis: Example:
Chlorpromazine.-Granulomatous
hepatitis. These granulomas are always non-caseating, intralobular or portal or both. They may be clinically silent. They may produce elevation of serum alkaline phosphatase due to small multifocal parenchymal compressions affecting the bile flow.Drugs involved:
Allopurinol, Aspirin, Diazepam, Isoniazide, Phenitoin, Sulphonamides.Steatosis,macrovesicular:
Presence of single, large fat droplets in hepatocytes pushing the nucleus to the periphery of the cell, with or without necrosis (pyknosis). This change is probably due to impaired egress of lipid from hepatocyte. The cell cannot export any more its lipoproteins.Drugs involved:
Glucocortocoids, Methotraxate, L-Asparaginase.Steatosis, microvesicular: presence of small fatty vesicles filling the cytoplasm of the hepatocyte (foamy hepatocyte). The nucleus is in the center of the cell. The lesion is attributed to interference with oxidation of fatty acids by mitochondria. Very serious lesion. Seen in azotemia, pancreatitis and acute steatosis of pregnancy. Some responsible drugs are: Tetracycline, Pirprophen, Amineptin, Valproate.
Phospholipidosis:
there are foamy hepatocytes plus, under electron microscopy, large lysosomal inclusions composed of densely packed concentric membranes with a fingerprinting pattern. There is also reduction of the crystae in the mithochondria and vesicles in the smooth ER. The lesion was recognized by Oda in Japan in 1969. Later, in 1975, it was recognized by Lullman et al in inborn errors of phospholipid metabolism. Drugs responsible: Colargil (Oda et al. 1969), Amiodarone (Pousell et al.1984).-Vascular lesions
: venous thromboses, necrotizing angiitis, arterial intimal hyperplasia,perisinusoidal fibrosis (Vit.A), sinusoidal dilatation, peliosis, veno-occlusive disease,
Budd-Chiari syndrome, hepatoportal sclerosis, nodular hyperplasia of the liver.
Drugs:
Immunosuppressive drugs, oral contraceptives, testosterone.-Hepatic tumors
: hepatocellular adenoma and carcinoma, cholangiocarcinoma, angiosarcoma, hemangioendothelioma.Drugs:
Anabolic and contraceptives drugs, Vinyl Chloride.
EXAMPLES
|
HALOTHANE HEPATITIS |
Click on picture to enlarge
Case History
Forty four year old lady hah uterine curettage for metrorrhagia. Eight weeks later she had hysterectomy. Three days after hysterectomy she became jaundiced. Seven days later she died in liver failure. Halothane was used as anesthetic in both surgical procedures. The autopsy showed massive liver necrosis. It appears that the liver damage was mediated by an immunoreactive mechanism. Multiple exposures increase the incidence of liver damage.
 |
Fig.8-4-1:Fulminant
halothane Hepatitis.
The liver is flabby, soft, friable similar to any acute viral hepatitis. It was called in the past "acute yellow atrophy".
|
|
AMIODARONE HEPATITIS |
Click on picture to enlarge
This drug may cause damage of the liver together with thyroid dysfunction, pulmonary fibrosis, neuropathy, skin discoloration, ecchymoses and corneal deposits. The toxicity is dose related and occurs with more than 200mg daily. The changes in the liver consist of phospholipidosis and alcoholic-like changes with Mallory bodies in periportal hepatocytes and late periportal fibrosis.The accumulation of amiodarone in the liver can be assessed by computerized tomography because of the high iodine content of the drug. Its iodine is responsible for the thyroid dysfunction. Mild increase of serum transaminases are seen in 15 to 55% of patients
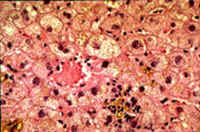 |
Fig. 8-4-4 Amiodarone hepatitis 54 year old male taking amiodarone for many years developed clinical hepatitis: ALT 780, AST 339. This slide demonstrates hydropic swelling of hepatocytes, focal cell necrosis with inflammatory reaction and cytoplasmic cholestasis. TheReview of Pathology of the Liver:Table of Contents foamy appearance is due to phospholipidosis present practically in every case and is due to accumulation ofsphingomyelin in hepatocytes. (see Em Picture below). |
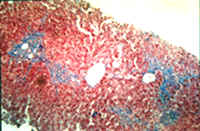 |
Fig.8-4-6. In this case, there is beginning portal, periportal andporto-central fibrosis. The case is lonstanding, more than 8 years under amiodarone treatment. |
|
Phenytoin (Dilantin) This anticonvulsivant drug which commonly causes lymphadenopathy, polyarteritis nodosa and bone marrow damage more rarely causes cinical hepatitis. Here it can cause cholestasis multifocal necrosis, lymphocyte "beading"in sinusoids similar to infectious mononucleosis but more commonly it causes multiple histiocytic granulomas which cause high elevation of serum alkaline phosphatase.
|
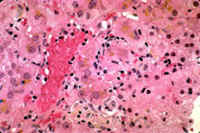 |
Fig. 8-4-7. Dilantin hepatitis.
This slide shows cytoplasmic cholestasis and sinusoidal beading of lymphocytessimilar to a mild case of infectious mononucleosis
|
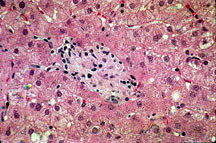 |
Fig. 8-4-8. Same case. Presence of a large Histiocytic granuloma, sharply demarcated, without necrosis. Tese histiocytic nodules act as mahy small space-occuping lesions wich compress the surrunding liver parenchyma afecting the bile flow thus producing retention of enzymes normally eliminated in the bile such as alkaline phosphatase
|
METHOTREXATE
|
Methotrexate The changes produced by this drug in the liver, in order of progressive severity, are: steatosis, ballooning degeneration, cell necrosis, nuclear changes, cholestasis, Ito cell hyperplasia, portal inflammation, progressive fibrosis, cirrhosis. Liver damage is directly related to DURATION of therapy and inversely related to the LENGTH OF INTERVALS between doses. Daily small doses are more dangerous than weekly large doses. The treatment must be monitored with repeat liver biopsies.There are no good alternatives to liver biopsies. Biochemical tests are insufficient for assessing the hepatic injury. |
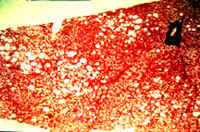 |
Fig. 8-4-9. Methotrexate hepatitis. This is the earliest lesion. Thre are foci of macrovesicular steatosis.
|
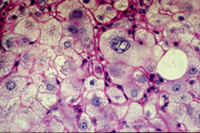 |
Fig. 8-4-10. Another case, advanced lesion.In this case the lesion is more advanced: there id ballooning degeneration, cellnecrosis, nuclear changes, fine cholestasis and beginning fibrosis,
|
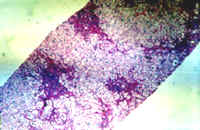 |
Fig.8-4-11. Another case, Late lesion. Besides the above illustrated cellular changes, in this case there is fibrosis, portal, periportal and porto-portal in some areas. |
| IV TETRACYCLINE CAUSING MICROVESICULAR STEATOSIS |
|
GRANULOMATOUS HEPATITIS |
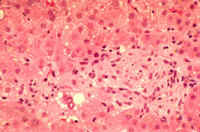 |
Fig. 8-4-13. Granulomatous hepatitis. This slide is from a patient treated with sulpha drugs. There is an intralobularhistiocytic granuloma, non- caseating.
|
|
VENO-OCCLUSIVE DISEASE |