li-11-6
PRIMARY SCLEROSING CHOLANGITIS
by Dr. E. Orfei
Definition
Progressive
non-specific chronic inflammation and fibrosis of intrahepatic and
extrahepatic bile ducts, of unknown etiology.
Similar
changes are produced by the secondary sclerosing cholangitis of known etiology.
At
difference with primary biliary cirrhosis which affects small intrahepatic bile
ducts, namely, interlobular and septal ducts, this disease affects bile
ducts of all sizes not necessarily at the same time, indeed it can be confined to
only intrahepatic ducts (Small duct disease) or only to large hepatic and
extrahepatic ducts (Large duct disease) or it may involve large and small
ducts simultaneously (Global disease). Also the gall bladder may involved in the in this
inflammatory and fibrotic process.
History
First
recognized by Delbet in France in 1924 and described as "Irregular
Fibrosis and Stenosis of the Biliary Tree", to be distinguished from
Secondary Sclerosing Cholangitis.
Clinical
features
The
clinical course is highly variable. In symptomatic cases the disease is
progressive and cause biliary cirrhosis with deeply green livers.Cholangitis and
Colangioarcinoma are often present.
Probably
asymptomatic cases in this disease are more frequent than it is suspected.
The
first symptoms are similar to those of PBC: progressive fatigue, pruritus and
jaundice in repeated episodes. The onset is therefore insidious and the disorder
is usually diagnosed 1-2 years after onset of symptoms. The full picture
of cholangitis, pain, fever and jaundice, is rare. most patients present
hepatosplenomegaly or jaundice.
Sex:
Prevalent in man (75% of cases).
Age:
2-75 years. Pick 25-45 years.
Associated
diseases: Inflammatory bowel disease, thyroiditis, pancreatitis, arthritis,
celiac sprue, sarcoidosis. Up to85% of patients with PSC have inflammatory bowel
disease, especially chronic ulcerative cholitis. Crohn's disease is rarely
associated. An individual with inflammatory bowel disease and high serum
alkaline phosphstase most likely has PSC. Symptomatic patients may live up to 15
years. Long term life is unlikely even for asymptomatic cases.
Laboratory
tests
Increased
serum alkaline phosphatase, transaminase, bilirubin and IgM. Mitochondrial
antibodies: rarely present.
Cholangiography:
Alternating strictures and dilatations and beading of intra and extraheptic bile
ducts. In cholelithiasis the ducts are dilated but not stenosed and beaded.
Pathogenesis
The
cause of PSC is unknown. Most likely the cause is a disorder of the immune
system. Specific immunologic markers such as antimitochondrial and
anti smooth muscle antibodies
are
largely absent. Frequent, however, is the association of PAC with HLA-B8 and
HLA-DR3 aplotypes.The lymphocytes that are involved in the inflammatory exudate
in affected bile ducts are T-lymphocytes. These immunologic alterations may have
a familial distribution.
Pathology
The
pathologic picture is that of a fibrosing obliterative cholangitis but the
histological findings are not specific for PSC.
There
is thick concentric clean fibrosis around bile ducts with degeneration of bile
duct epithelium and transformation of bile ducts into fibrous cords.These
fibrous changes are seen in 40% of cases. Rarely the fibrosis affect only
intrahepatic bile ducts.
In
large ducts, such as extrahepatic and primary intrahepatic ducts, the fibrosis
is so thick with young plump fibroblasts replacing the disappeared ducts as to
simulate a fibrosarcoma or
a Clatchkin tumor. In interlobular and septal ducts the fibrosis is wide
and clean of inflammatory cells. Instead of fibrous changes some portal areas
show inflammation and disappearance of bile ducts. The inflammation consists of
lymphocytes, plasma cells, neutrophils and periductal edema. The typical
florid duct lesion that is seen in PBC is not seen in PSC. Periportal
cholestasis and granulomas may be present. These finding demonstrate that the
distinction between PSC of small ducts and PBC is morphologically possible
only in 28% of cases.
The
liver biopsy especially in early cases is not distinctive,
therefore when the disease is suspected endoscopic retrograde cholangiography
must be done. The positivity of this test with negative Anti-Mitochondrial
Antibibodies will establish the diagnosis.
Illustrations
|

Fig.11-6-1.
Large ducts fibrosis. This section is from the hilus of the liver
deeply green, cholestatic, in a 32 year old male who had PSC of
extra and intrahepatic bile ducts. He died within 2 years of acute
cholangitis following surgery.
Sections
of the white cords in this specimen were diagnosed fibrosarcoma by very
renowned pathologists.
|
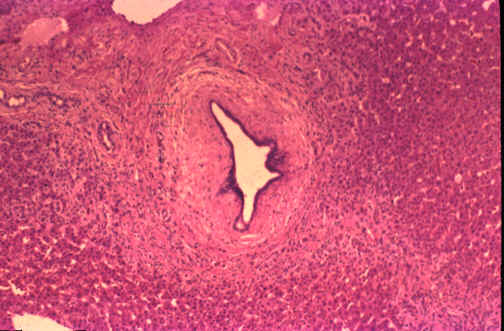
Fig. 11-6-2. Septal duct .
This
is a septal duct in the previous case. Notice marked periductal
fibrosis. Normally septal ducts have a fibrotic cuff.
In
this case the fibrosis is excessive.
|
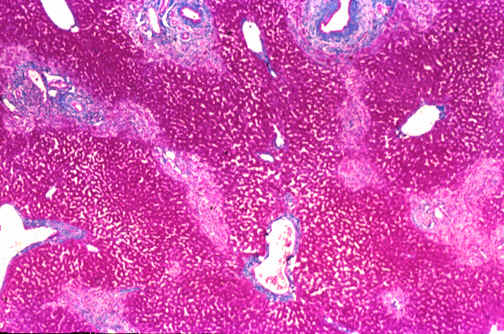
Fi11-6-3. Small duct fibrosis fibrosis.
In
this case notice the portal , periportal and bridging fibrosis
originating
from periductal fibrosis. Cirrhosis in this disease and in biliary
obstruction in general develops very slowly over a long period of time. These
livers will be large and green.
|
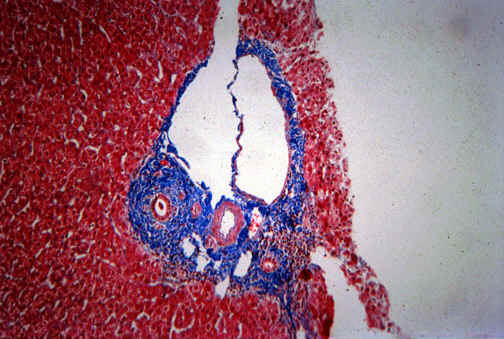
Fig. 11-6-4. Portal duct fibrosis.
This is a portal field with a typical PSC obtained by liver
biopsy. The cholangiography confirm the diagnosis.
|
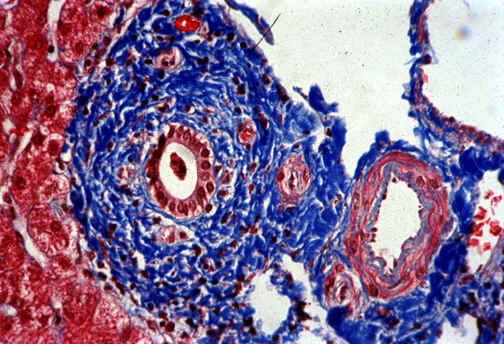
Fig.
11-6-5. Portal bile duct.
High
power of previous picture.
Notice
the rather clean periductal fibrosis. Although very clear , this change is
not specific for PSC, which must be confirmed by cholangiography.
|
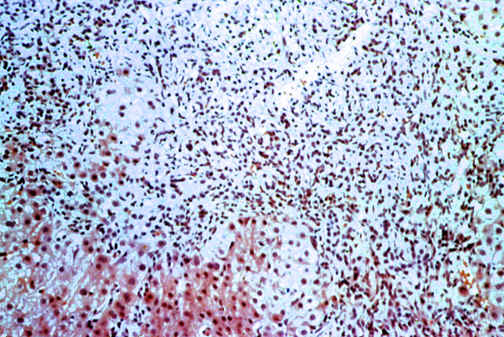
Fig. 11-6-6. Portal
inflammation. Unusually PSC
may cause
chronic portal inflammation Characterized by disappearance of portal
bile ducts.
|
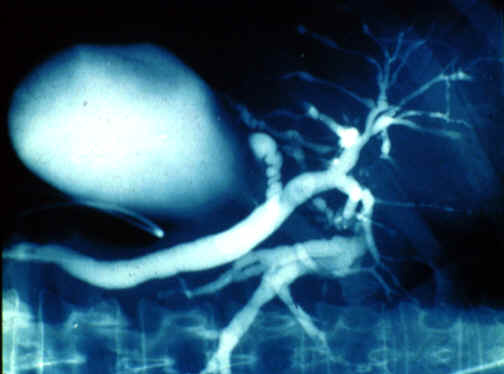
Fig.11-6-7. Cholangiogram in PSC. Stenoses,
dilatations and beading of intrhepatic ducts are the
diagnostic features in a case of clinically and morphologically
suspected for PSC.
|
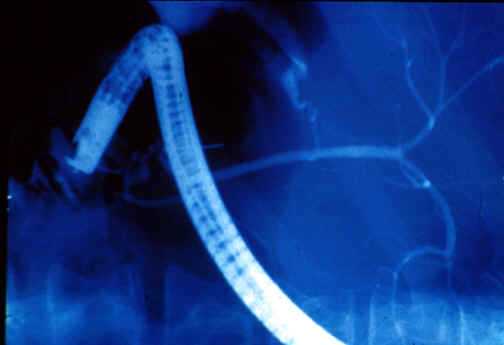
Fig. 11-6-8. Normal Xray
of
intrahepatic bile duct branches.
|
TO CONTENTS/ TO
VANISH







